Aarogya Care | 5 min read
Is the Cost of the COVID-19 Test Covered Under Health Insurance Plans?
Medically reviewed by
Table of Content
Key Takeaways
- COVID-19 can affects anyone but older people are at greater risk
- Health insurers provide COVID-19 hospitalization and treatment cover
- Ayushman Bharat Yojana provides free health cover to the poor and needy
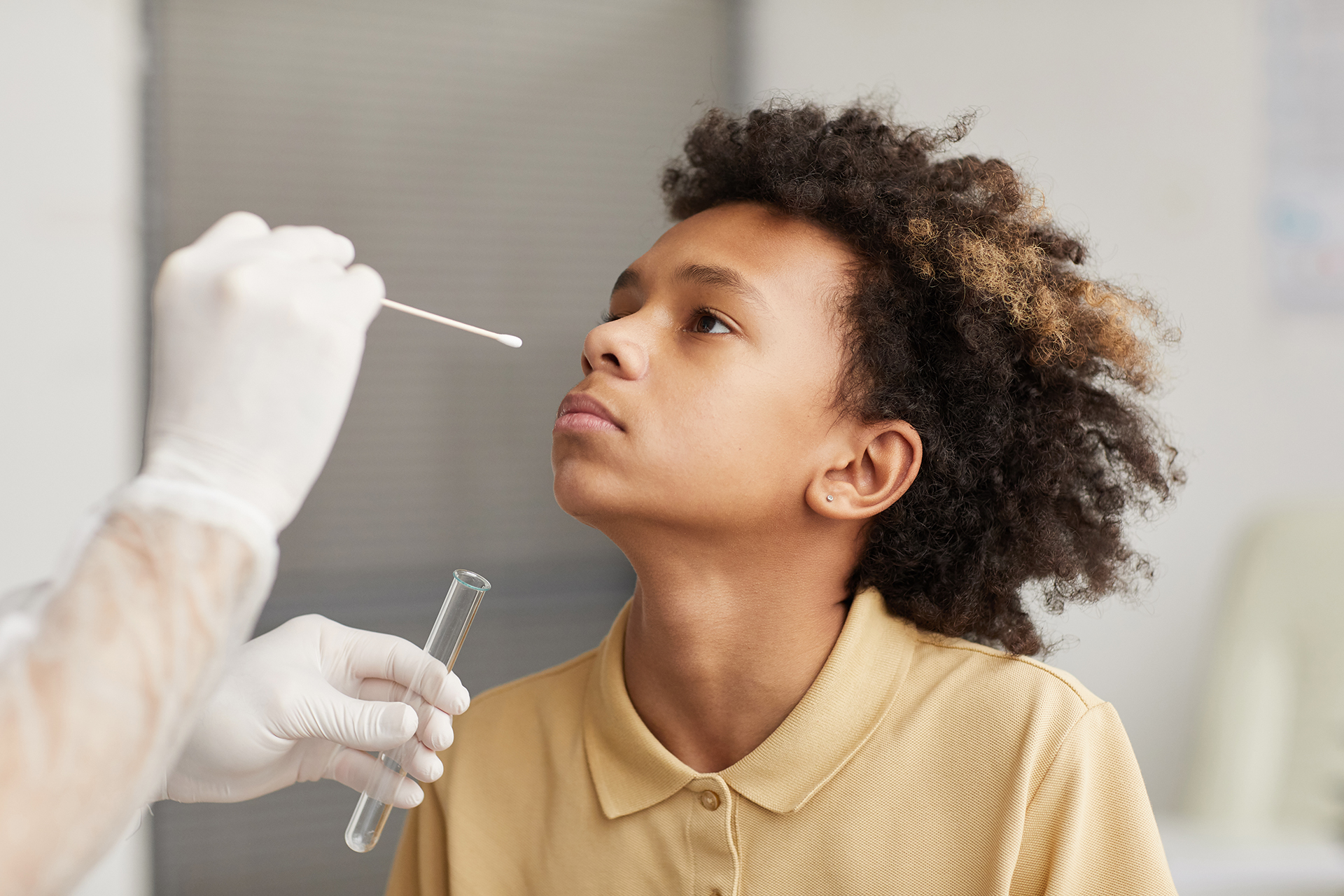
COVID-19 is a contagious disease that has taken the world by storm [1]. The novel coronavirus mostly affects older people and those with existing medical conditions when compared to children and younger people. It is extremely vital for you to get tested for the disease if you experience any symptoms or come in contact with an infected person.
What’s more, medical inflation is on the rise and accessing care can be costly. Health insurance does act as a savior during difficult times [2]. But does health insurance cover the costs of COVID 19 test? Getting the test done at private hospitals and diagnostic centers can become a costly affair. Read on to know how to get tested without financial worries.
How to Get a Free COVID 19 Test Done in India?
Apart from spreading awareness about precautionary measures to prevent the spread, the Government of India is taking steps for the safety of people. It has made testing for COVID-19 free of cost at government hospitals and laboratories. In case you or your loved ones have any symptoms of the novel coronavirus, call the toll-free COVID-19 helpline number. Inform about your symptoms to know if you need to get tested. If there is a need, you can visit government-approved labs near you and get tested for free.
If you are visiting a private hospital for COVID 19 tests and treatment, you will have to bear the costs from your pocket. However, if you have an existing health insurance plan, you can get the treatment costs reimbursed from your insurer. This way, you can get the COVID-19 test done for free. The IRDAI has advised health insurers in India to include COVID-19 hospitalization and treatment costs.
Additional Read: COVID-19 Facts
How Much Do Private Labs and Clinics Charge for COVID-19 Tests?
Certain private laboratories and diagnostic centers have been authorized to conduct COVID-19 tests. However, private labs and hospitals charge you fees for the testing. In April 2020, private health institutes charged a maximum of Rs. 4,500 per head. This included a screening test for Rs. 1,500 and a confirmation test for Rs. 3,000. As a large portion of India’s population can’t afford the expenses, the ICMR made private labs and hospitals charge subsidized rates.
Later in the year, private labs and hospitals across the country reduced the COVID-19 test charges by a good margin. The fees for the COVID-19 testing now vary for different states. For instance, a maximum of Rs. 2,400 is charged in New Delhi. The rates in Maharashtra are set at Rs. 2,200 to Rs. 2,800. Likewise, private hospitals charge Rs. 2,000 to Rs. 2,500 in UP and up to Rs. 3,000 in Tamil Nadu. The government of Karnataka has capped the COVID-19 testing prices at Rs. 2,500 while West Bengal has lowered the prices by 45%.Do Health Insurance Companies Cover COVID-19 Testing?
According to the IRDAI, all health insurance companies will provide COVID-19 hospitalization and treatment cover. Even regular, indemnity-based health policies cover COVID-19 tests as part of pre-hospitalization expenses subject to certain conditions. Your existing health insurance policy is sufficient. You do not require a special COVID-19 health policy to cover the cost.
Ensure you buy a health insurance policy that provides adequate cover to you and your family. But, remember that your insurer will only reimburse the cost of the COVID-19 test if you are tested positive and are hospitalized for at least 24 hours. The COVID-19 diagnostic test is covered under the health plan if it was done up to 30 days before hospitalization. To make it simple, a regular health insurance plan will cover COVID-19 related hospitalization and diagnostic tests under pre and post-hospitalization cover if you are tested positive.
Do Health Insurance Policies Cover the Cost of the COVID-19 Test done at Home?
Most of the COVID-19 indemnity-based health plans include home treatment expenses. However, not all health insurance plans may cover it. Most policyholders with ‘Corona Kavach’ and ‘Corona Rakshak’ plans can claim home care treatment expenses for COVID-19. This includes medication, doctor’s fee, CT scan, x-ray, and other specific tests. Note that these expenses are covered under COVID-19 specific plans.
It is important to inform your insurer at the earliest if you are tested COVID-19 positive and are undergoing treatment at home. However, you need to submit a few documents to claim coverage towards home treatment. This includes a COVID-19 positive test report from an ICMR-approved testing lab and a doctor’s prescription for home isolation and treatment.
Additional Read: Health Insurance During Pandemic a Safe SolutionWhat is Ayushman Bharat Pradhan Mantri Jan Arogya Yojana?
Ayushman Bharat Pradhan Mantri Jan Arogya Yojana (AB-PMJAY) is an initiative by the Government of India to provide the poor and needy with a health cover against COVID-19 [3]. Under this cover, testing and treatment for COVID-19 are free for poor people living in rural and urban areas. This includes:
- Laborers
- Rickshaw pullers
- Ragpickers
Such individuals benefit from this scheme and have free access to testing and medical treatment at private and government network hospitals. This step is taken by the government to provide timely healthcare to the underprivileged.
How to File a Claim for COVID19 Test Expenses?
Claiming a settlement claim for COVID-19 expenses is similar to any other regular health insurance claim. Keep all your hospitalization and test bills ready with you. You can opt for a cashless claim if you get treated at a network hospital. Submit your documents at the earliest if filing for reimbursement. Looking at the present pandemic situation, insurers now accept claim applications over email. Simply self-attest the bills, scan, and email them.
When you buy a health insurance policy, select the plan that provides you with both illness and wellness benefits. Consider buying Complete Health Solution plans offered by Bajaj Finserv Health. These plans offer you and your family a medical cover of up to Rs. 10 lakh along with various benefits. This includes preventive health check-ups, reimbursement on consultations, network discounts, and more.
References
- https://www.who.int/news/item/13-10-2020-impact-of-covid-19-on-people's-livelihoods-their-health-and-our-food-systems
- https://www.livemint.com/market/mark-to-market/indias-already-stiff-healthcare-costs-get-a-pandemic-boost-11621582098264.html
- https://www.pib.gov.in/PressReleasePage.aspx?PRID=1738169
Disclaimer
Please note that this article is solely meant for informational purposes and Bajaj Finserv Health Limited (“BFHL”) does not shoulder any responsibility of the views/advice/information expressed/given by the writer/reviewer/originator. This article should not be considered as a substitute for any medical advice, diagnosis or treatment. Always consult with your trusted physician/qualified healthcare professional to evaluate your medical condition. The above article has been reviewed by a qualified doctor and BFHL is not responsible for any damages for any information or services provided by any third party.