General Physician | 7 min read
Impetigo: Symptoms, Causes, Contagious, Complications
Medically reviewed by
Table of Content
Synopsis
Impetigo is a common skin infection that is contagious and results in blisters and sores. The bacteria Staphylococcus aureus or Streptococcus pyogenes are impetigo causes. It can be treated by applying prescription mupirocin antibiotic ointment or cream to the sores.
Key Takeaways
- There are three types of impetigo based on the bacteria that causes impetigo and the sores it produces.
- Maintaining a clean workplace and maintaining good personal hygiene are essential to treating and preventing impetigo.
- Impetigo causes little threat, although it can occasionally lead to scarring, cellulitis, and kidney issues.
You may feel panicked if you discover a rash or blisters on your child's skin. But before you assume the worst, these sores may be brought on by impetigo, a bacterial skin infection that, when treated, is often harmless. However, it is a contagious bacterial infection. Although adults can also contract it, newborns and small children are most commonly affected.
Impetigo can be contracted by touching a person with it and their sores, mucus, or nasal discharge. Sharing personal items like towels, clothes, and other belongings with sick persons can also spread impetigo. It might appear frightening, but it's not necessarily painful, and the available treatments can get rid of it very quickly.
Additionally, you can be more vulnerable if you: Reside in a tropical area with hot, humid summers and mild winters, suffer from scabies infection, participate in sports or hobbies where cuts and scrapes are frequent or live in a crowded environment or close quarters. People who live in the same home or children who attend daycare frequently get infections.
How Does Impetigo Occur?
Bacteria can enter the skin after being bitten, scratched, or given a wound that opens the skin, leading to an impetigo infection. But even if the skin is not damaged or perforated, it can still spread there. Impetigo occurs more frequently in the warmer months when kids are outside more. Usually, the first indications of impetigo are sores and blisters on the lips and nose. Legs and arms may also develop impetigo.
Impetigo Symptoms
Depending on the bacterium that causes it and the sores it causes, impetigo symptoms is divided into three types. Each type progresses in a certain way.
1. Non-bullous Impetigo
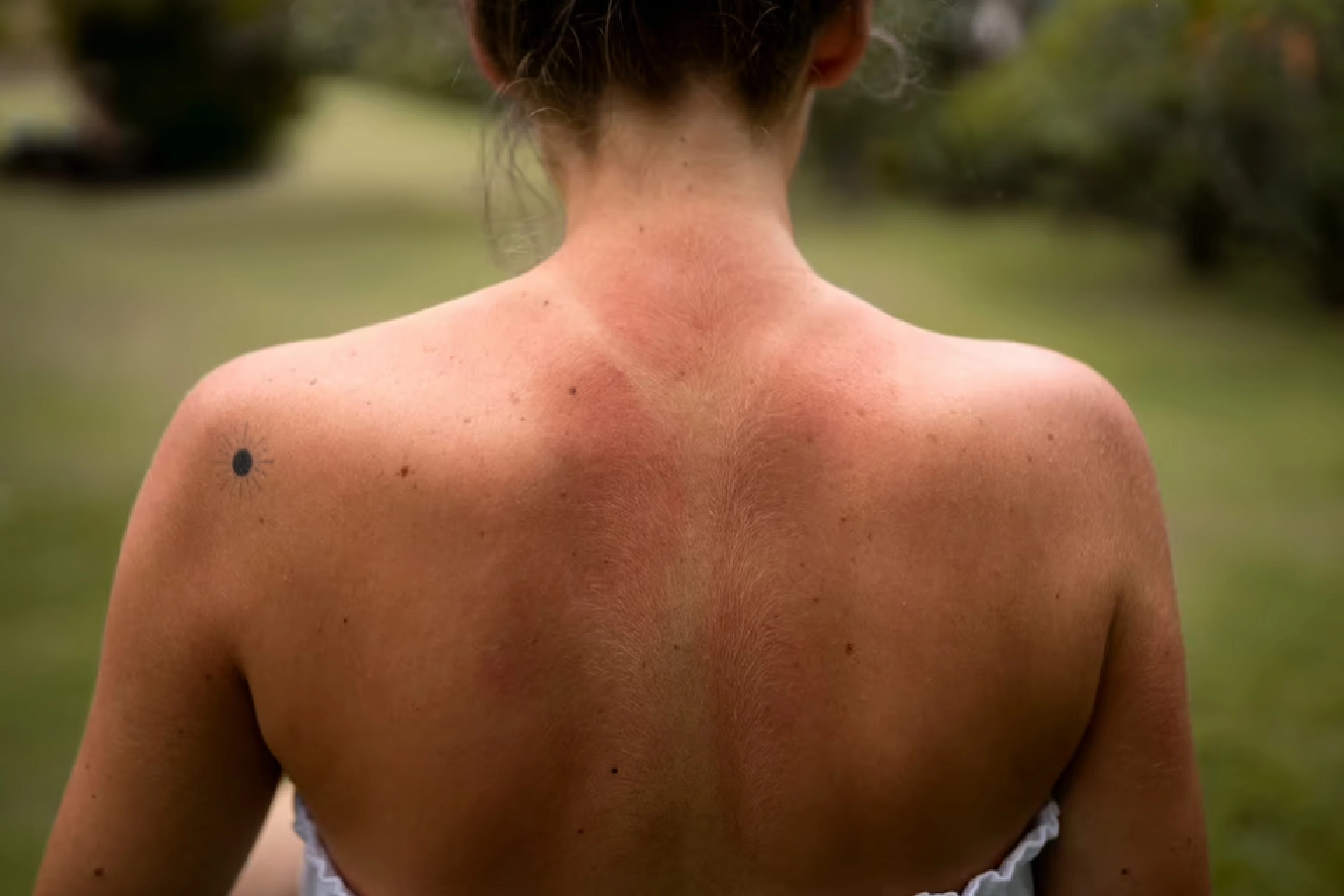
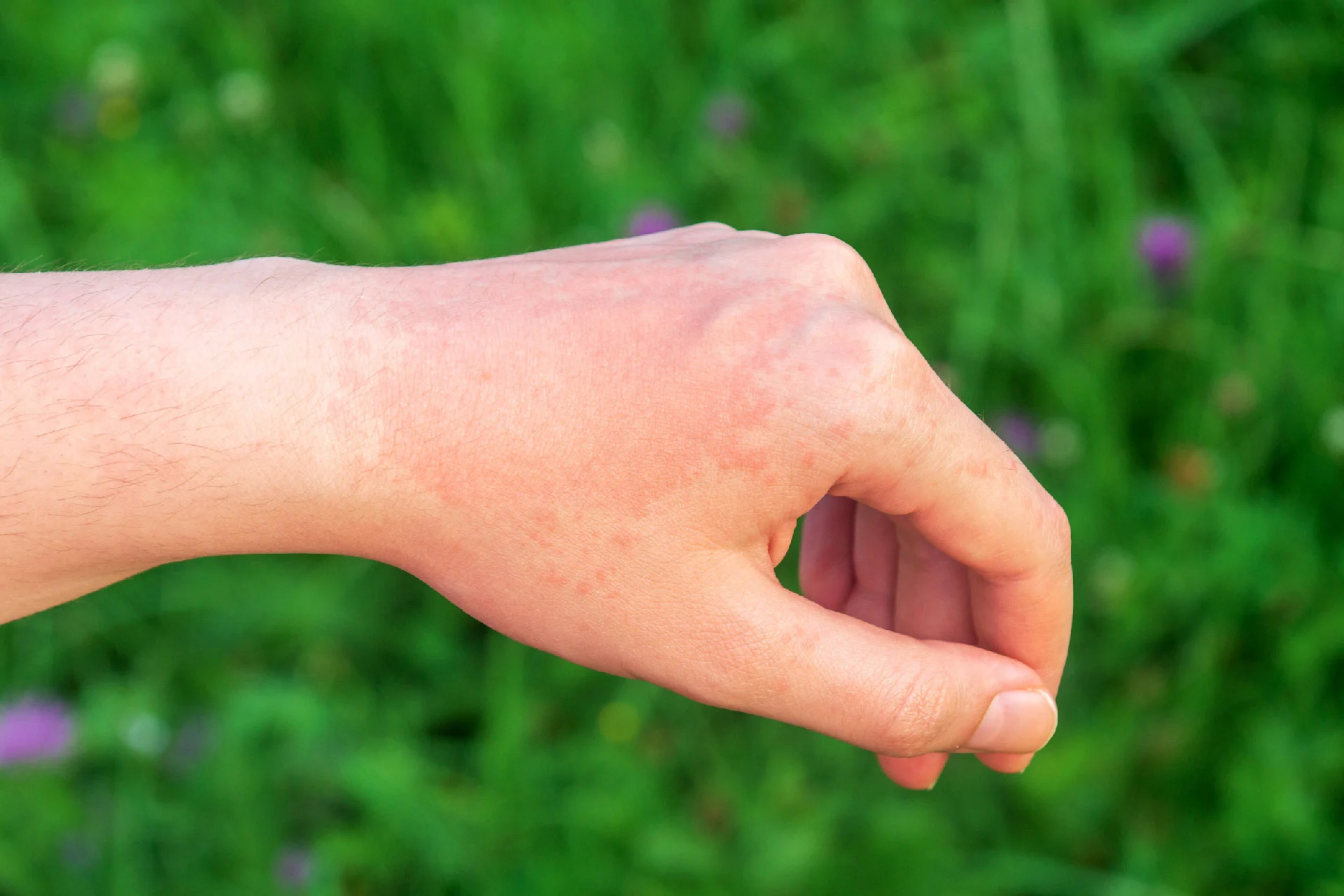
The first non-bullous impetigo symptoms are red sores, which typically form around the mouth and the nose but can also affect other parts of the face and limbs. The sores immediately break, leaving behind 2 cm wide, thick, golden crusts. The crusts create a red stain after drying, but it usually goes away without leaving any scars. It can take anywhere from a few days and a few weeks for the redness to go away. The sores don't hurt, but they could itch. Avoid touching or scratching the sores to prevent the illness from spreading to other body areas.
Fever and swollen glands are two more symptoms that are uncommon but might appear in more severe cases.

2. Bullous Impetigo
Bullae, which are fluid-filled blisters that typically form on the central region of the body between the waist and neck or on the arms and legs, are the first sign of bullous impetigo. The blisters typically measure 1-2 cm in diameter.
The blisters could grow swiftly before bursting a few days later, leaving a yellow crust that often heals without any scars. The skin around the blisters may itch, and the blisters themselves may hurt. Therefore, avoiding touching or scratching the skin's affected areas is crucial, just like with non-bullous impetigo. Feverish symptoms and swollen glands more frequently accompany bullous impetigo.
3. Ecthyma
This far less common and much more severe infection can occur if impetigo is left untreated. In addition, due to its deeper skin penetration, ecthyma is a more severe form of impetigo than other forms.
The infection results in uncomfortable blisters on the feet, ankles, thighs, and legs. As time passes, the blisters develop into thicker-crusted, pus-filled ulcers. And frequently, the skin around the sores turns red. Ecthyma sores may leave scars and take a very long time to cure.
Additional Read: Staph Infection TreatmentImpetigo Causes
It can be caused through either the staph infection-causing Staphylococcus aureus bacteria or the group A streptococcus bacteria, which also causes strep throat.
The top layer of skin can become infected by bacteria if they enter the body through a wound. You are vulnerable to impetigo after any skin damage. This includes minor wounds like cuts and scrapes. Insect bites also increase impetigo risk.
Impetigo Risk factors
- Children between 2 and 5 are most likely to get impetigo.
- It is easily spread through skin contact in sports, in crowded places like schools and daycare centers, and within families.
- Hot and muggy weather makes it more probable for impetigo infections to spread.
- Impetigo bacteria typically enter the skin by a small cut, an insect bite, or a rash.
- Other medical conditions - Children with other skin conditions, such as atopic dermatitis, are more likely to develop impetigo (eczema skin).
- Additionally, older people, diabetics, and those with weakened immune systems are more likely to develop it.

Impetigo Contagious
It can occasionally appear even if the skin is unharmed. Close contact with someone with an active infection increases your risk because this skin condition is highly contagious.
Direct skin contact and sharing toys, blankets, and towels are effective ways to spread it. However, because of this, impetigo can spread more quickly in crowded places like daycare centers.
If your kids participate in sports that require skin contact, they are also at risk. These activities may include football and wrestling. These infections are more common in the summer and tropical areas because the bacteria can survive in warm, humid conditions.
Swimmers are also at risk, especially if they contact an infected object or use a towel shared by someone with this bacterial skin infection.
Impetigo Diagnosis
A medical professional can determine if you have impetigo based on how the sores appear. A skin sample may be collected by the clinician and sent to a lab. The correct antibiotic can be used if pathologists can identify the bacteria that is causing the illness.
Impetigo Treatment
1. Maintain the House Clean
Everyone in the household should clean the same way, even if only one person has impetigo. Regularly wash with soap and water. This should help in the treatment of mild infections. The patient should consult a doctor if this doesn't help. They might have to take medication on prescription.
2. Topical Antibiotics
Mupirocin ointment, which can only be obtained with a prescription, works well in treating mild infections. Soak the wounds in warm water, then gently scrape away any scabs to allow the antibiotic to penetrate the skin. Staph and strep infections cannot be treated with antibacterial creams that are available over-the-counter. If there are recurrent breakouts, the dermatologist will recommend an antibiotic ointment for every person in the house. It will eradicate the bacteria in the nose.
3. Oral Pills
The doctor may prescribe antibiotics to be taken orally if the patient has ecthyma or many impetigo sores. Ensure care to take the medication to the end, even if the sores have healed.
Additional read: Skin Polishing TreatmentImpetigo Complications
The most frequent side effects of impetigo, though they are uncommon, are as follows:
Cellulitis happens when a bacterial infection damages the tissue beneath the skin and spreads to the bloodstream and lymph nodes. This can become fatal if it is not treated.
Take immediate action instantly if there is a skin wound to avoid cellulitis. Apply a preventive topical ointment to the wound each day to prevent infection. Get doctor consultation if you exhibit early indications of a skin infection, such as increasing pain, redness, or blistering.
Some strep germs that cause impetigo can also induce glomerulonephritis. Blood in the urine and high blood pressure are two signs of this inflammatory kidney disease.
Rheumatic fever and post-streptococcal glomerulonephritis are very uncommon consequences of impetigo. However, if this consequence exists, it often develops one to two weeks following the healing of the skin lesions.
Can impetigo be Prevented?
The best ways to avoid getting sick are to maintain good health. However, to prevent impetigo, you can also:
- Keep your hands tidy by constantly washing your hands. If you don't have soap and water, sanitize with an alcohol-based product. Practice regular skincare, such as exfoliating your skin, or try skin polishing treatment.
- Maintain proper hygiene by frequently trimming your (and your child's) fingernails to prevent scratching. Use a tissue to catch your sneeze, then discard the tissue. Take a bath every day, especially if your child has sensitive or eczema skin.
- Please keep your child from scratching any cuts, scratches, or wounds they may receive.
- Cover sores to stop the bacterium that causes impetigo from spreading to other parts of the body or other people.
- Cuts, scratches, and other wounds should be cleaned with soap and warm water, then treated the wound with an antibiotic cream or ointment.
- Wash sheets, towels, and undergarments in hot water to keep clothes clean.
References
Disclaimer
Please note that this article is solely meant for informational purposes and Bajaj Finserv Health Limited (“BFHL”) does not shoulder any responsibility of the views/advice/information expressed/given by the writer/reviewer/originator. This article should not be considered as a substitute for any medical advice, diagnosis or treatment. Always consult with your trusted physician/qualified healthcare professional to evaluate your medical condition. The above article has been reviewed by a qualified doctor and BFHL is not responsible for any damages for any information or services provided by any third party.