Dermatologist | 5 min read
Melasma: Definition, Causes, Types, Symptoms and Treatment
Medically reviewed by
Table of Content
Key Takeaways
- Melasma is of three types, dependent on the depth of the pigmentation
- Melasma on face can appear on cheeks, jawline, nose, forehead, and upper lip
- Melasma treatment includes certain creams, topical steroids, and procedures
What is Melasma? it is a common skin condition that causes discolored and dark patches on your skin. Owing to its high prevalence during pregnancy, nearly 15-50% [1], melasma is also often known as the ‘mask of pregnancy. Another lesser-known word for melasma is chloasma. Melasma in men is not as common as in women. According to research, the condition affects women 9X more than men. The most effective melasma treatment combines sun protection with medications.
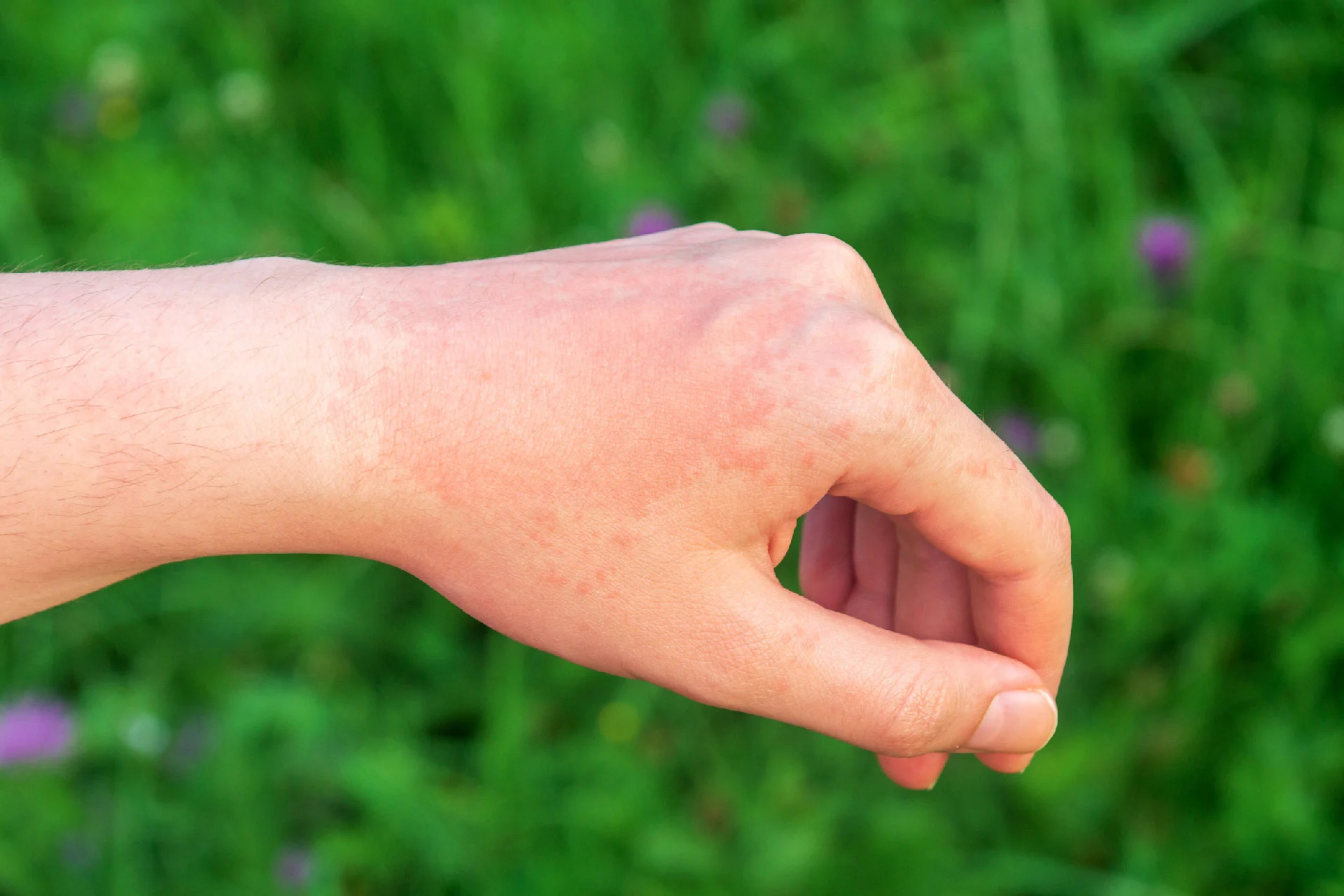
Melasma usually darkens and lightens over a period of time. Often, the condition may get worse during summer and better during winter. Melasma looks like gray, blue, light or dark brown freckles or flat patches. Areas that are commonly affected by this condition are the face and forearms. It can appear on your forehead, upper lips, or cheeks. Despite being harmless, having visible melasma on your face can make you feel self-conscious or anxious in public spaces.
Read on to understand the types, symptoms, and cause of melasma as well as melasma treatment options.
Melasma Types
The type of melasma you have depends on the depth of the pigmentation. Usually, the black light of a Wood lamp can help determine this. Here are the common types of melasma.
Epidermal
This type of melasma is usually brown and may also have a well-defined border. Its appearance is generally obvious under a black light. Epidermal melasma usually responds well to treatment.
Dermal
In case of dermal melasma, the discolored patches on your skin will generally have a bluish or light brown color. It also has blurry borders. Generally, dermal melasma doesn’t respond well to prescribed treatment.
Mixed
This is the most common form of melasma and has both, brownish and bluish patches. When seen under a black light, this type appears to have a mixed pattern. Mixed melasma responds to the treatment prescribed to some extent.
Additional Read: Home Remedies for SunburnSymptoms of Melasma
Hyperpigmentation is a primary sign of melasma. If you have it, your skin loses its color or its tone becomes uneven. This type of melasma may typically be darker than your skin tone and is usually flat. Patches of melasma are generally pain-free but may make your feel uncomfortable.
Usually, melasma on face covers the following areas.
- Nose, cheeks, upper lip, and forehead: Also known as centrofacial
- Cheeks: Also known as lateral cheek pattern, where the patches are visible on both cheeks
- Jawline: Also known as mandibular
- Cheek and nose: Known as malar
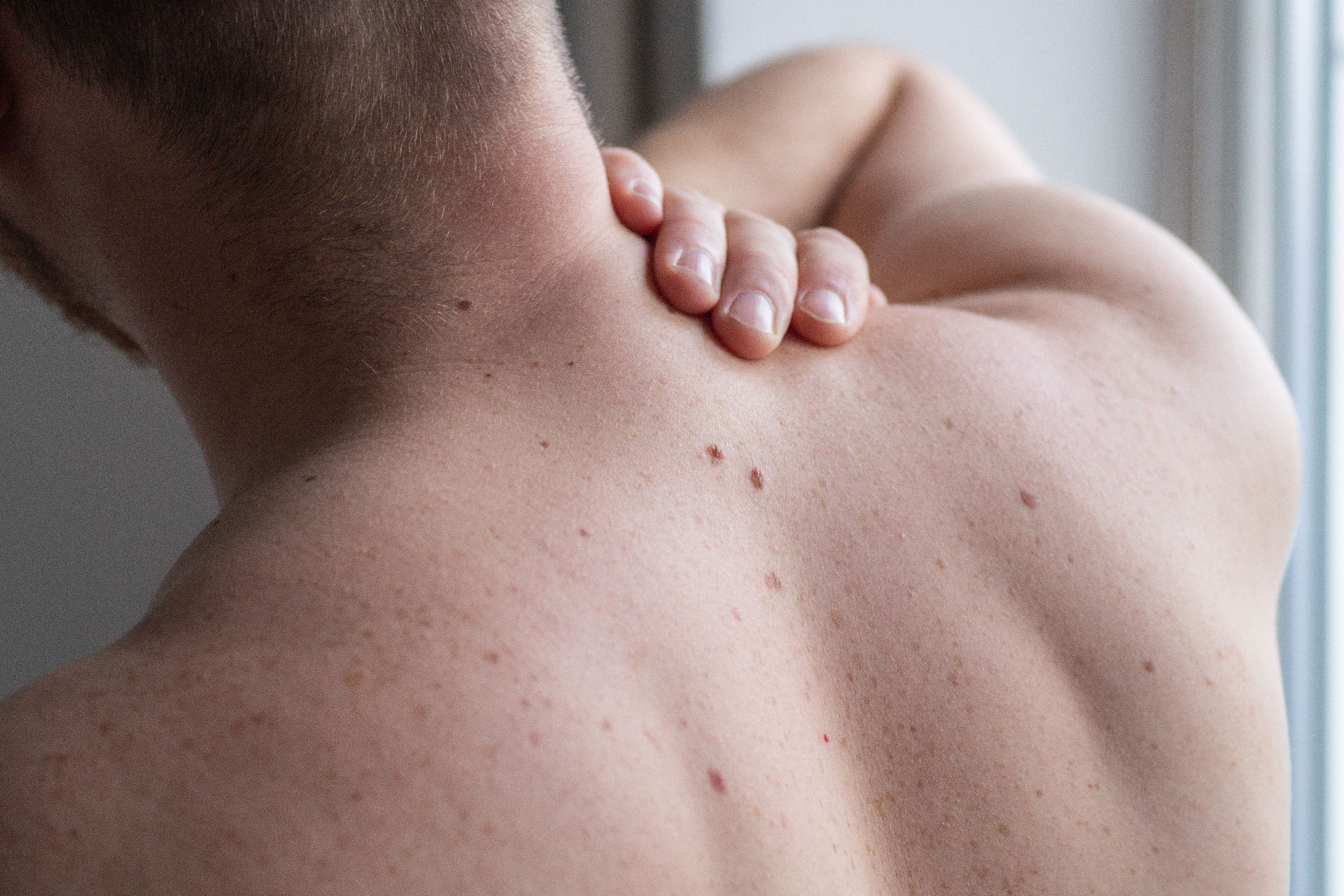
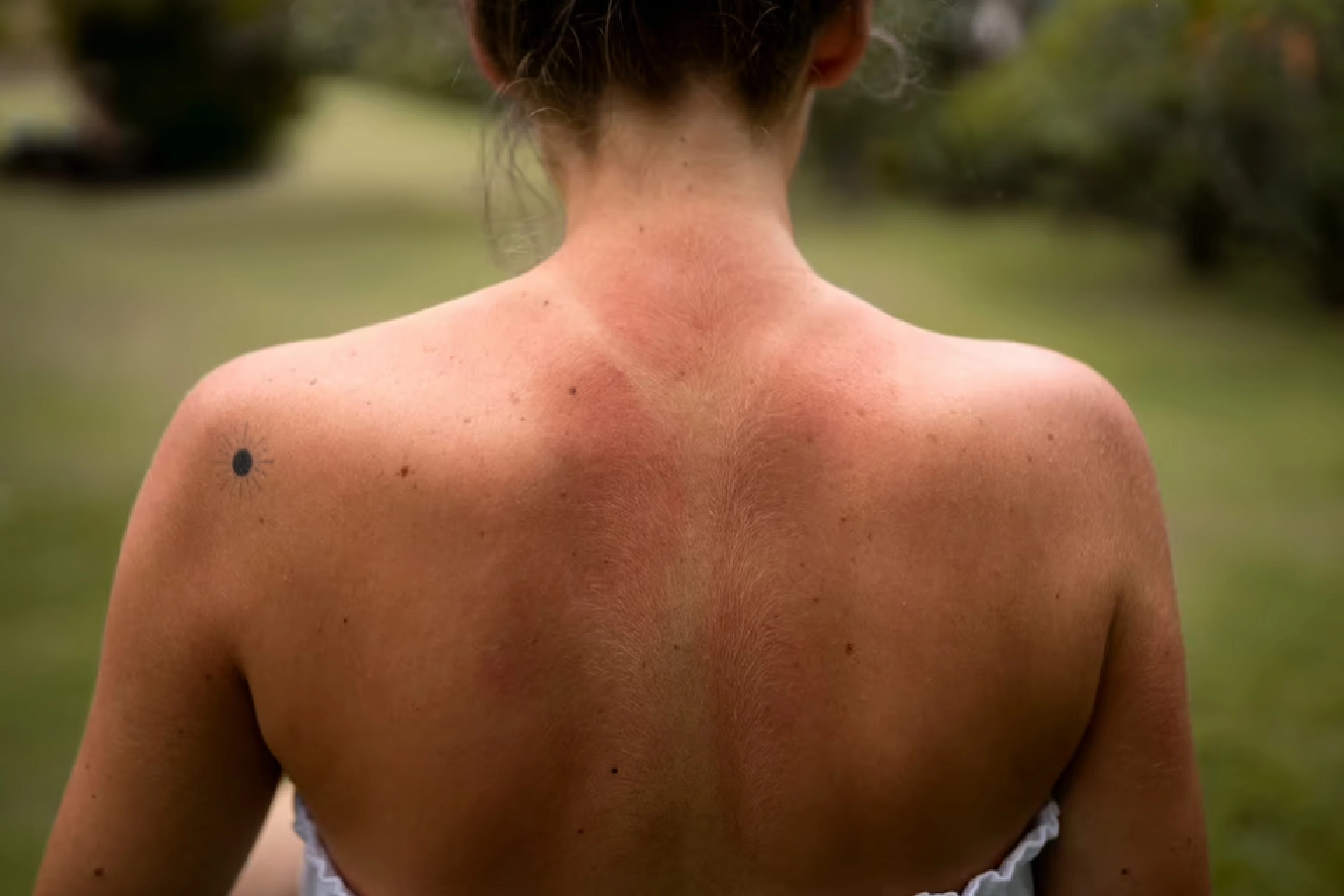
In rare cases, melasma can also appear on your neck, upper arms and shoulders. Melasma on upper arms and shoulder is also known as brachial melasma. Melasma on neck generally appears in people over the age of 50 [2].
The best way to know if you have melasma is to consult a doctor as soon as you see the signs. Your dermatologist can help you get an accurate diagnosis and form a melasma treatment plan. If needed, you doctor may also advise you to get a biopsy to help diagnose the condition.
What Happens Inside our Skin?
The largest organ in your body, the skin, is an organ that accounts for around one-seventh of your total body weight. Your barrier is made of your skin. As a result, your bones, muscles, organs, and everything else are shielded from the elements, bacteria, sunlight, dampness, toxins, injuries, and more. Also, it aids in maintaining a healthy body temperature, guards against dehydration, and allows you to detect sensations like the warmth of a stove and the pressure of another person holding your hand.
Three layers make up your skin. The epidermis is the top layer, followed by the dermis in the middle and the subcutis at the bottom. Melanocytes, which are found in your epidermis, store and create the dark pigment known as melanin. Your skin darkens because the melanocytes create more melanin in response to hormone stimulation, light, heat, UV radiation, or hormonal stimuli.
How is Melasma Diagnosed?
Melasma is frequently diagnosed through a visual examination of the afflicted area. Your healthcare expert might also carry out some tests to rule out specific causes.
An examination with a Wood's lamp is one testing method. A unique form of light is held up to your skin in this manner. It enables your medical professional to examine your skin for fungal and bacterial infections as well as to assess how many layers of skin are affected by the melasma. They might also suggest a biopsy to look for any significant skin problems. For testing, a little piece of the damaged skin must be removed.
What are the Different Causes or Triggers for Melasma?
Melasma has two basic causes - hormones and radiation, including ultraviolet, visible, and infrared (heat) light. The sun's ultraviolet and infrared rays have a major role in aggravating melasma. Some potential melasma causes include:
- Anti-Seizure Drugs: Medicines that stop seizures could be a factor in the development of melasma. For example, Clobazam
- Contraceptive Therapy: Melasma has been seen in those who take oral contraceptives that contain progesterone and oestrogen (contraceptive medication, birth control)
- Diethylstilbesterol: A synthetic (man-made) version of the hormone oestrogen, also known as Diethylstilbesterol, is frequently employed in the treatment of prostate cancer. Once more, there is a correlation between elevated oestrogen levels and melasma
- Genetics: Between 33% and 50% of those who have melasma say that a family member also has the condition. Melasma is common in identical twin pairs [1]
- Hypothyroidism: Your thyroid being underactive can be another cause of melasma
- LED screens: The LED lights from your tablet, phone, laptop, and television may contribute to Melasma
- Pregnancy: It is unknown why pregnant women experience "the mask of pregnancy." According to specialists' theories, the elevated amounts of oestrogen, progesterone, and melanocyte-stimulating hormones during the third trimester of pregnancy may play a part [2]
- Hormones: In certain people, hormones like progesterone and oestrogen may be involved. It has been noted that postmenopausal women who take progesterone in the form of a pill or any other way can develop melasma. Your melasma lesions most likely include higher than average amounts of oestrogen receptors, even if you aren't pregnant
- Cosmetics: Cosmetics can cause a phototoxic reaction in some women
- Phytotoxic drugs: There are several antibiotics, nonsteroidal anti-inflammatory drugs (NSAIDs), diuretics, retinoids, hypoglycaemics, antipsychotics, targeted therapies, and other medications that are phototoxic (make you sensitive to sunshine)
- Skincare items: A substance that generally irritates your skin will probably aggravate your melasma
- Soaps: It's believed that some perfumed soaps can worsen or bring on melasma
- Tanning beds: The UV radiation produced by tanning beds can sometimes be even more damaging to your skin than the UV light from the sun
![What causes Melasma]()
How is the Melasma Treated?
Melasma can go away naturally when there are changes in the diet or lifestyle. For example, it can go away after delivery for women suffering from it during pregnancy. Also, if a woman takes birth control pills, it can go away once they stop consuming them. However, for it to work, these hormonal changes caused by pregnancy or birth control pills should be the cause of melasma. Sometimes, physicians also recommend sunscreen with high SPF to get rid of melasma.
Some, on the other hand, may experience melasma for years or possibly the remainder of their lives. A person can seek treatment to help eliminate or diminish the patches if melasma does not go away on its own with time.
Even after a successful course of treatment, melasma may recur since not all treatments are effective for everyone. The following are some possible melasma treatments:
Aloe Vera Gel
Aloe vera has a gentle, deeply hydrating, and moisturising nature. It nourishes and shields the skin from the damaging effects of UV exposure by rehydrating dry skin and penetrating deeply into the skin's layer. It has been demonstrated that aloe vera helps pregnant women with melasma.
Turmeric
Turmeric is a well-known anti-inflammatory, antioxidant, and antimutagenic compound. It can be used as a homemade DIY skin treatment for melasma, and you can also add gramme flour and milk to create a nourishing scrub or mask.
Black Tea
Tea's natural astringent properties are very moisturising and help to soothe and calm inflammation-related pigmentation. Apply steeped black tea to dark melasma patches on your face using a cotton ball.
Medical/Health Care Procedures
In the event that topical treatments are ineffective, a dermatologist might advise:
- Laser therapy
- Chemical peeling
- Microdermabrasion
- Light treatment
- Dermabrasion
Several of these treatment approaches can have negative side effects or lead to new skin issues. It is best to discuss potential hazards with a physician or dermatologist.
If someone has previously experienced melasma, they can strive to avoid triggers by reducing exposure to the sun, wearing a hat outside, and using sunscreen.
Melasma Treatment Options
The best treatment for melasma on face, neck, upper arms, or anywhere else is to make sure that the condition does not worsen. In order to do so, avoid all the possible triggers. If you are in the sun for a long period, use a sunscreen that contains iron oxide and has an SPF of 30-50. Make sure to apply it after every two hours and wear a hat that has a wide brim.
Your doctor may also prescribe creams or a topical steroid that can help lighten the areas affected by melasma. Doctors may also advise you to get dermabrasion, chemical peels, or microdermabrasion. These melasma treatment options work by removing the top layers of your skin to lighten the patches. In rare cases, there is no option to lighten the patches.
Keep in mind that even after successful treatment, melasma can reappear. In order to reduce the chances of reappearance, go for regular visits and follow the skin practices prescribed by your doctor. You can also try ayurvedic skin care home remedies but be sure to talk to the doctor before taking any steps.
Additional Read: How to Treat RosaceaWhat are the Risk Factors Pertaining to Melasma?
The exact cause of melasma is unclear. However, those with darker skin are more vulnerable than those with pale skin. The disease is also linked to sensitivity to oestrogen and progesterone. This implies that melasma can be brought on by hormone therapy, pregnancy, and birth control pills.
The causes of melasma are also known to include stress and thyroid disorders.
Sun exposure can also result in melasma because UV rays harm the cells that regulate pigment (melanocytes).
Risk factors include the following:
- Exposure to Sun: Melasma might develop if you are exposed to UV radiation frequently
- Skin tone: Those with light brown skin tones are more likely to get melasma, especially if they dwell in regions with extensive sun exposure
- Female Gender: About nine times more women than men are affected with melasma [3]
- Pregnancy: Melasma affects 15% to 50% of pregnant women, making it more prevalent at this time. Hormones related to pregnancy may be to blame [4]
- Genetics: Up to 50% of melasma sufferers claim that their immediate family members also have the disease [5]
Possible Causes of Melasma Include:
- Pregnancy-related hormone changes (chloasma)
- Hormone therapy
- Using birth control pills
- Sun exposure
- Some skin care products that irritate the skin
- Some medications, such as anti-seizure drugs and those that make the skin more sensitive to sun exposure, like retinoids, blood pressure drugs, and some antibiotics
How is Melasma Cured?
In order to cure melasma properly, your healthcare professional first need to find the cause behind it. There are multiple reasons behind melasma, for example, contraceptive pills, hormonal imbalance etc. When the root cause is identified, it can be cured easily without any issues.
Depending on the individual, melasma may go away on its own, be permanent, or react to treatment within a few months. However, most melasma cases will go away over time, especially if you protect yourself well from sunshine and other light sources.
Regrettably, melasma cannot be permanently removed with a single therapy. However, you can avoid the things mentioned below if you have melasma:
- Hormone therapies, particularly those that use oestrogen
- Birth control, specifically oestrogen- and progesterone-containing oral contraceptives
- Led light from your tablet, phone, laptop, and television
- Makeup that makes your skin uncomfortable
- Drugs that can worsen or cause melasma
- Fragranced soaps
- Goods for skincare that make your skin itch
- Tannery tables
- Waxing, which could make melasma worse
Melasma can mimic other forms of hyperpigmentation and skin conditions including cancer. Because of these characteristics of melasma, it is important to get an accurate diagnosis and treatment. Book a teleconsultation or in-clinic appointment with top dermatologists on Bajaj Finserv Health as soon as notice any symptoms, be it of melasma, hives on skin, or any other condition. This way, you can get treated at the right time and protect your skin.
References
- https://www.ncbi.nlm.nih.gov/books/NBK459271/
- https://my.clevelandclinic.org/health/diseases/21454-melasma#
Disclaimer
Please note that this article is solely meant for informational purposes and Bajaj Finserv Health Limited (“BFHL”) does not shoulder any responsibility of the views/advice/information expressed/given by the writer/reviewer/originator. This article should not be considered as a substitute for any medical advice, diagnosis or treatment. Always consult with your trusted physician/qualified healthcare professional to evaluate your medical condition. The above article has been reviewed by a qualified doctor and BFHL is not responsible for any damages for any information or services provided by any third party.