Physical Medicine and Rehabilitation | 6 min read
Pityriasis Rosea Rash: Causes, Symptoms, Complications
Medically reviewed by
Table of Content
Synopsis
Pityriasis rosea may seem like a hard name to pronounce. It is nothing but rose-colored scale that appears like a rash. It is not a life-threatening condition but having proper awareness about it is crucial.
Key Takeaways
- Pityriasis rosea is a commonly seen benign skin rash and is not life-threatening
- Pityriasis rosea is not contagious, and its exact causes are still unknown
- Pityriasis rosea symptoms are fairly easy to treat, and they usually resolve on their own
We have gathered all the information and statistics you need about Pityriasis rosea symptoms to help you understand the basics of this condition. However, getting a doctor’s opinion before doing anything that can potentially affect your health is wise.
What is Pityriasis Rosea?
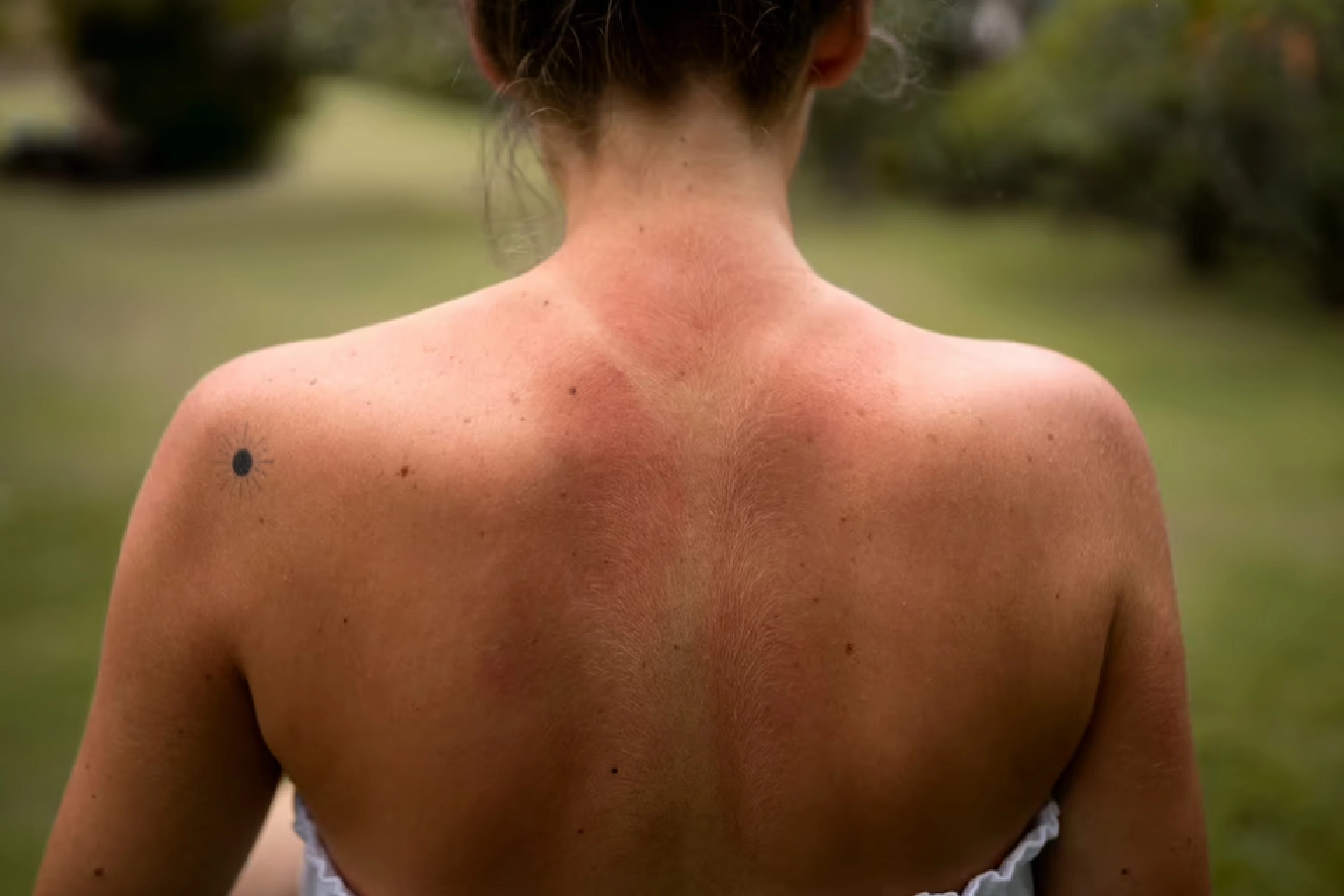
Pityriasis rosea is a skin rash usually found on the chest, abdomen, back, upper arms, and legs. It was first seen in 1860 [1]. It is a condition where inflammation of the dermis causes red itchy patches to form, resulting in a bit of discomfort. These rashes typically go away without intervention within a few weeks. But unfortunately, there is not much you can do to prevent it from occurring in the first place either.
Pityriasis rosea first presents itself as an oval scaly plaque called a herald patch and is then followed by many other small rashes. It is also known by some other names, such as Pityriasis circinata, herpes tonsurans maculosus, and roseola annulate.
Pityriasis rosea is a non-contagious benign skin condition. It will not spread to anyone around you and is non-cancerous. It is harmless but just a hassle to deal with. More examples of such skin conditions are skin tags. But unlike Pityriasis rosea, they require skin tag removal to get rid of and don’t go away on their own.
The most commonly affected groups are teenagers and young adults between the ages of 10 to 35, but it can happen to people of any age. It is also seen more often in women than men.
Around 0.5 to 2% of people develop Pityriasis rosea once in their lifetime and never get affected by it again. But it is not impossible to develop the condition more than once. Studies have shown that in only 2% to 3% of people, Pityriasis rosea has recurred. So if you ever get this skin condition, you probably won’t have to worry about dealing with it again.
Moreover, other forms of Pityriasis rosea also exist. These may be different in regard to the shape, size, distribution, or symptoms. Some examples include versicular Pityriasis rosea, purpuric Pityriasis rosea, and many more. It is primarily why a diagnosis can be made only by a professional by seeing the lesion. Even then, many doctors do run additional tests.
How to Check Pityriasis Rosea?
Pityriasis rosea symptoms first starts with a single red scaly patch on your torso called a “mother patch” or “herald patch.”
After a week or two of the appearance of the mother patch, smaller red rashes called “daughter patches” begin to form. These rashes often resemble the shape of a Christmas tree and start to itch, especially when exposed to heat or sweat.
If you have Pityriasis rosea, you will see a similar pattern in the progress of your rashes and might experience some of the following pityriasis rosea symptoms.
Additional Read: Prickly Heat Rash
Common Pityriasis Rosea Symptoms
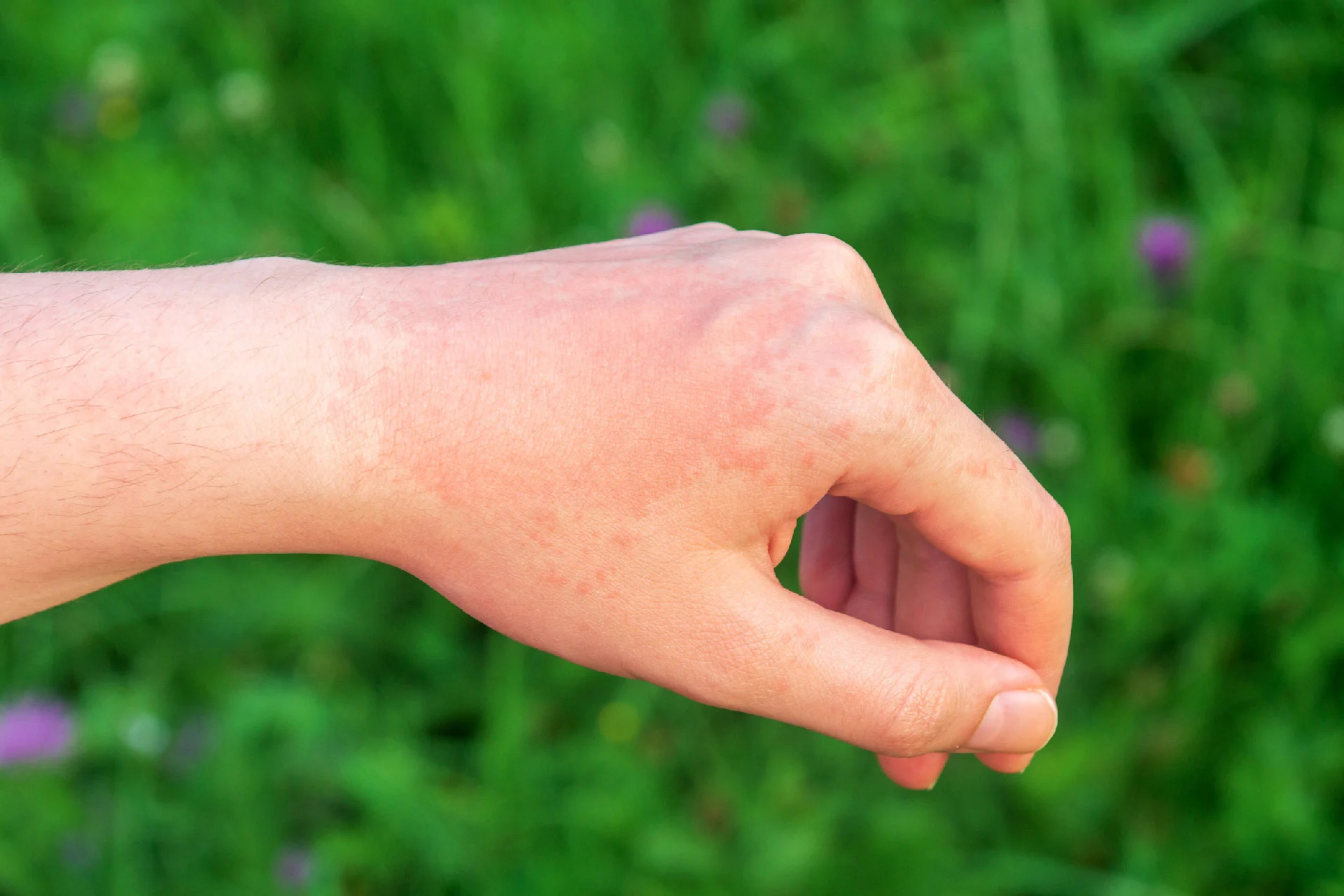
- Oval patch of about 2 to 10 cm in diameter
- Red raised and rough in texture rashes
- Itching
- Gastrointestinal disturbance
- Headache
- Fever
- Sore throat
- Fatigue
- Joint pain
Pityriasis Rosea Causes
Doctors are uncertain of the condition’s origin. Most incidents can be linked to seasonal variations or infections, but the exact cause is still unclear.
- Seasonal variations are considered one of the causes as Pityriasis rosea occurs more frequently in spring and winter.
- It is important to note that barely some people who got Pityriasis rosea in the past have developed it again. This suggests that they became immune to the condition. These signs all point to the potential cause being an infection.
- Recently, studies also showed that 8-69% of patients that suffered from upper respiratory tract infections also developed Pityriasis rosea [2]. The study’s results strengthen the argument that Pityriasis rosea is caused by an infectious agent.
- Other speculations of Pityriasis rosea causes are drug-induced reactions or vaccines.
Despite the big list of potential causative agents and research, doctors have not seemed to come to conclude what exactly causes Pityriasis rosea.
Additional Read: Winter Rash: Diagnose, Treatment
Pityriasis Rosea Diagnosis and Treatment
A dermatologist usually performs a physical examination to rule out any other skin condition. The examination involves simply observing the rash.
They may order a blood test, a scraping, or a biopsy to collect a sample tissue, ruling out other skin conditions such as eczema, tinea versicolor, or a biopsy to confirm it is indeed what they suspect ringworm and psoriasis. Pityriasis rosea is self-limiting, which means it resolves on its own. Rashes usually clear up within five to eight weeks in most patients. In others, it can take just 45 days or up to five months or longer.
To help with Pityriasis rosea symptoms or in severe cases, a doctor may recommend:
- Over-the-counter topical medications – zinc oxide or calamine lotion
- Antihistamines – a medicine prescribed for allergies, rashes, or itching
- Corticosteroids – prescription drugs to lessen swelling
- Antiviral medication – to counter herpes viral infection
- Hydrocortisone cream – to deal with the itching sensation
- Light treatment – UV rays are believed to reduce the rash duration
It is important to note that each medication has its own side effects. For example, UVB phototherapy may leave behind dark spots, which will fade over time.
The type of Pityriasis rosea treatment prescribed will depend on the individual and vary according to their condition. A doctor should oversee treatment to avoid further health complications.
These home remedies may help relieve discomfort:
- Take a lukewarm oatmeal bath
- Apply a moisturizer or lotion
- Avoid heat and keep yourself cool
- Apply sunscreen with at least SPF 30
- Get some natural or artificial sunlight
What to Avoid Pityriasis Rosea?
- Scratching
- Soaps with fragrances
- Hot water
- Heat
- Exercising
- Sweat
- Wool
- Synthetic fabrics
The factors mentioned above are some irritants that can make Pityriasis rosea rashes worse.
Additional Read: How Is Rosacea DiagnosedPityriasis Rosea Complications
In most cases, Pityriasis rosea doesn’t return after it goes away, and the complications are not as severe if you have no underlying health conditions.
Pityriasis rosea complications in some cases include:
- Spots that remain after rashes heal
- Intense itching (in 25% of patients)
If the rashes last for more than three months, it may be because of your body’s reaction to certain medications. Pregnant women have a higher chance of serious complications resulting from this condition. Some studies show Pityriasis rosea onset during pregnancy can lead to birth complications, premature deliveries, and miscarriages. If you are pregnant and are suffering from this skin condition, consult your obstetrician as soon as possible.
Will My Skin Go Back to Normal?
Pityriasis rosea does not leave marks or scars after it goes away. However, skin discoloration may persist for 6 to 12 months, but eventually, the skin will return to normal.
If you have any spots left after the rashes, go away or after UVB phototherapy, you can try a skin polishing treatment that gently exfoliates the skin and diminishes the appearance of dark patches.
Pityriasis rosea is not a skin condition you need to worry much about. It does not affect those around you and goes away before you even know it. You'll indeed feel better if you try self-care remedies and avoid irritants. First, however, you must talk to a doctor to get the guidance you need to recover faster. With the help of Bajaj Finserv Health, you can now book an online doctor consultation and speak with a dermatologist to get answers to all your skin-related queries. This is especially useful if you have a skin condition like Pityriasis rosea and are required to stay away from the harsh sun and are supposed to wear comfortable clothing.
References
- https://emedicine.medscape.com/article/1107532-overview#:~:text=Pityriasis%20rosea%20(PR)%20is%20a,psoriasis%2C%20and%20Pityriasis%20rubra%20pilaris.
- https://pubmed.ncbi.nlm.nih.gov/6849825/
Disclaimer
Please note that this article is solely meant for informational purposes and Bajaj Finserv Health Limited (“BFHL”) does not shoulder any responsibility of the views/advice/information expressed/given by the writer/reviewer/originator. This article should not be considered as a substitute for any medical advice, diagnosis or treatment. Always consult with your trusted physician/qualified healthcare professional to evaluate your medical condition. The above article has been reviewed by a qualified doctor and BFHL is not responsible for any damages for any information or services provided by any third party.